A 63-year-old woman presented with an acute exacerbation of chronic back pain after a fall. She was taking warfarin because of a history of factor V Leiden, deep vein thrombosis, and pulmonary embolism, for which a temporary inferior vena cava (IVC) filter had been placed 8 years ago. Her physicians had subsequently tried to remove the filter, without success. Some time after that, 1 of the filter struts had been removed after it migrated through her abdominal wall.
Laboratory testing revealed a supratherapeutic international normalized ratio of 8.5.
Magnetic resonance imaging of the lumbar spine showed a para-aortic heterogeneous collection, suspected of being a retroperitoneal hematoma (Figure 1).
Magnetic resonance imaging of the lumbar spine showed a para-aortic heterogeneous collection, suspected of being a retroperitoneal hematoma.
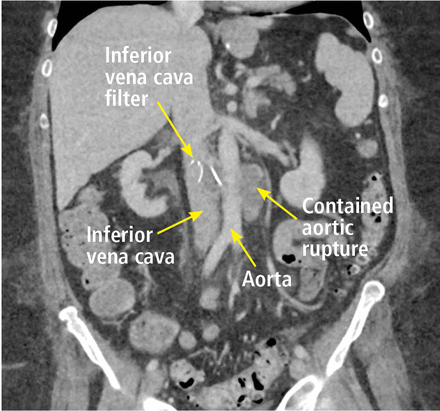
Computed tomographic angiography of the abdomen and pelvis subsequently revealed a contained aortic rupture, a filter strut within clotted blood adjacent to an aortic pseudoaneurysm, and additional filter struts within the second portion of the duodenum and renal pelvis (Figure 2).
Computed tomographic angiography of the abdomen and pelvis revealed a contained aortic rupture and inferior vena cava filter struts within clotted blood adjacent to an aortic pseudoaneurysm.
The patient underwent endovascular aneurysm repair with adequate placement of a vascular graft. She was discharged on therapeutic anticoagulation, and her back pain had notably improved.
COMPLICATIONS OF IVC FILTERS
In the United States, the use of IVC filters has increased significantly over the last decade, with placement rates ranging from 12% to 17% in patients with venous thromboembolism.1
The American Heart Association recommends filter placement for patients with venous thromboembolism for whom anticoagulation has failed or is contraindicated, patients unable to withstand pulmonary embolism, and patients who are hemodynamically unstable.2 While indications vary in the guidelines released by different societies, filters are most often placed in patients who have an acute bleed, significant surgery after admission for venous thromboembolism, metastatic cancer, and severe illness.3
Complications can occur during and after insertion and during removal. They are more frequent with temporary than with permanent filters, and include filter movement and fracture as well as occlusion and penetration.4,5
In our patient, we believe that the 3 remaining filter struts likely penetrated the wall of the IVC to the extent that they encountered adjacent structures (aorta, duodenum, kidney).
Of cases of IVC filter penetration reported to a US Food and Drug Administration database, 13.1% involved small bowel perforation, 6.5% involved aortic perforation, and 4.2% involved retroperitoneal bleeding. Symptoms such as abdominal and back pain were present in 38.3% of cases involving IVC penetration.5
Therefore, the differential diagnosis for patients with a history of IVC filter placement presenting with these symptoms should address filter complications, including occlusion, incorrect placement, fracture, migration, and penetration of the filter.4 If complications occur, treatment options include anticoagulation, endovascular repair, and surgical intervention.
Footnotes
Dr. Duggirala has disclosed a commercial interest as a consultant for EBSCO Health.
- Copyright © 2018 The Cleveland Clinic Foundation. All Rights Reserved.